Re-emergence of malaria
The deadly form of malaria, falciparum, has re-emerged on the Thailand-Myanmar border in the first half of 2023 undoing decades of highly effective elimination work. New strategies are needed to tackle this re-emergence to avoid deaths.
Previously malaria was diagnosed and treated at an early stage. However, the displacement of people and collapsing health services, due to the civil war since the military coup in 2021, have resulted in the re-emergence.
Malaria can be as easy to treat as a common cold but there are times when it is hard. Pregnant women and children are particularly vulnerable when infected.
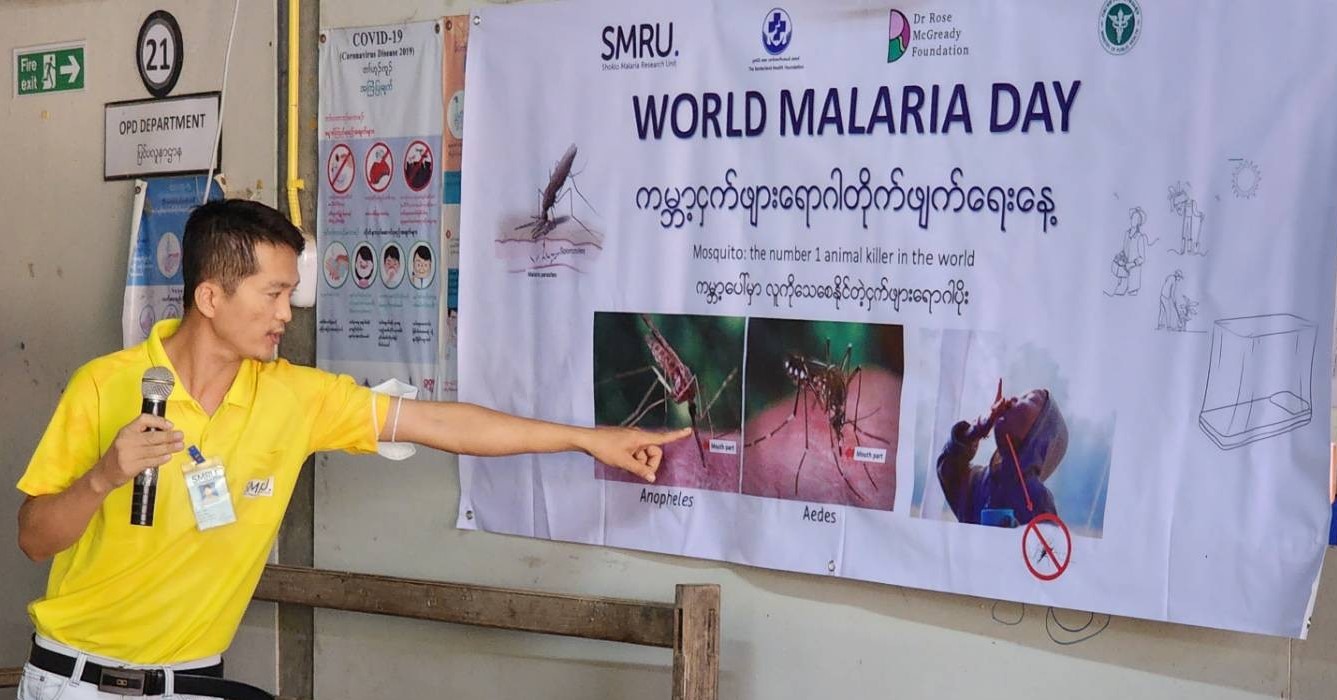
World Malaria Day is especially timely and important this year. The Foundation is proud to support Rose and her team, who are trusted health providers, to remind people to be wary of this deadly infection from mosquitoes through malaria information and awareness activities.
Access to accurate information is a major challenge because regular news has been cut and wordy pamphlets are ineffective because of poor health literacy, after years of underinvestment in education. Explaining malaria symptoms and recognising the mosquitoes that carry it are key prevention strategies. The mosquito colouring is relaxing but highly effective educational activity for all age groups.
Many adults may never have coloured a picture in their lifetime due to lack of pencils and paper.
Malaria in the clinic
Rose shares a typical story from the situation her team currently face.
Phone 20:00 hours, Rose gets a call from the clinic.
Medic: ThraMu has chills, fever 40 degrees, her pulse is too fast and she is 9 months pregnant. This is her first visit to the clinic because she lives too far and there has been fighting in her area. The foetal heart beat is 170 – it is fetal distress. We did the malaria smear and it is positive – she has vivax with high count and already has moderate anaemia. She is 49 kilograms.
Rose: What would you like to do?
Medic: Start treatment according to the guideline page 41.
Rose: That’s a good choice. I would also give her IV fluid for rehydration. Do you have an IV line? Is she making urine?
Medic: I will start IV line and check her urine output.
Rose: Does she have labor pain?
[mumble, ruffle, crackle …]
Midwife: ThraMu has strong contractions 3 times in 10 minutes. The cervix is 5cm, station is 0. FHB is distress. She is going to deliver soon.
Rose: Have you got a standby blood donor? Please prepare for haemorrhage.
Midwife: Yes. No. Yes, I will check husband and family for blood group and ask the staff.
Two hours later, the mother has delivered with haemorrhage and a blood transfusion is up and running. Her fever is down, the cord blood and baby are negative for malaria. After 3 days, everyone is okay. The mother is discharged with family planning prepared and a warning about the risk of malaria for the baby in this first month.
If an Australian woman finds out she is in the early stages of pregnancy and has malaria, because of travelling internationally to a malaria affected country her treatment will be evidence based. It will be safe to treat her with the same medication provided to non-pregnant women. This treatment relies heavily on the work done by Rose’s team where women face the risk of malaria every day. Read more here.